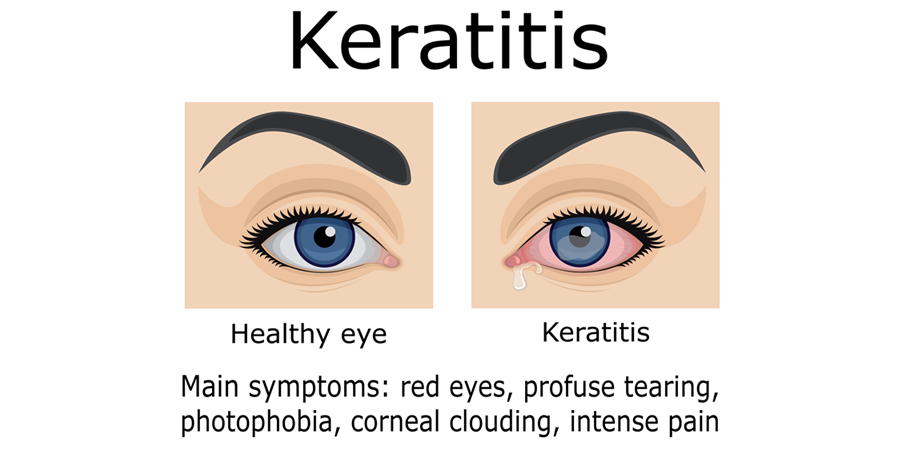
Keratitis refers to inflammation of the cornea, the clear, dome-shaped front surface of the eye that covers the iris and pupil. It may be infectious (caused by bacteria, viruses, fungi or parasites) or non-infectious (due to injury, dry eye, UV exposure, etc.).
Infectious causes:
• Bacterial organisms (especially in people who wear contact lenses)
Cleveland Clinic
• Viral infections, e.g. herpes simplex or shingles virus
• Fungal infections, often in agricultural or humid environments, or after injury with plant material
• Parasitic infections, particularly Acanthamoeba, which is a risk among contact lens users exposed to water.
Non-infectious causes:
• Eye trauma (scratch, foreign body)
• Poor contact lens hygiene, extended wear, or using lenses in water (swimming, etc.)
• Ultraviolet (UV) exposure
• Underlying conditions like dry eyes, eyelid problems, immune system disorders, or vitamin A deficiency.
Symptoms
Keratitis can present with several signs and symptoms. Some common ones are:
| Notes |
| Symptom | What the person might feel / see |
|---|---|
| Redness of the eye | The eye looks bloodshot or inflamed. |
| Pain, irritation, or a gritty feeling | Feels like something is in the eye. |
| Excess tearing or discharge | More watery or sometimes mucous- or pus-like discharge. |
| Blurred or reduced vision | Especially if the central cornea is involved. |
Also Sensivity to light – Bright light causes discomfort. Also this virus leaves scar marks in the cornea which can be permanent or superficial.
Treatment
Non-infectious:
• Remove cause (e.g. stop using contact lenses).
• Artificial tears / lubricants to reduce irritation.
• Anti-inflammatory drops in some cases.
Infectious: depending on the organism
• Bacterial: frequent topical antibiotics. May need strong or broad-spectrum drops. Possibly oral antibiotics if severe.
• Viral: antiviral eye drops, sometimes oral antivirals.
• Fungal: antifungal eye drops, possibly systemic treatment; tends to be slower.
• Parasitic: specialized treatment. These may be resistant, and treatment can be prolonged.
Surgery: If there’s severe damage, non-response to medicines, or scarring that threatens vision, corneal transplant or other surgical interventions may be considered.
Complications
If keratitis is not treated promptly or properly:
- Corneal ulceration and scarring, which may permanently reduce vision. P
- Perforation of the cornea in severe cases.
- Spread of infection to other parts of the eye.
Prevention
Some key preventive steps:
- Always follow proper contact lens hygiene: wash hands, use the correct solutions, avoid sleeping in lenses unless prescribed, avoid contact with water while wearing them.
- Protect eyes from injury: wear protective eyewear in risky environments.
- Avoid excessive UV exposure: wear sunglasses with UV protection.
- Treat dry eye, eyelid disorders, and maintain overall eye hygiene.
- Early treatment is essential in this form of disease.
When to See a Doctor
You should see an ophthalmologist (eye specialist) if you have:
- Eye redness + pain that doesn’t improve quickly with rest or basic care.
- Blurry vision
- Strong sensitivity to light which leads to severe headache and eye pain.
- Any discharge or signs of infection.
- History of contact lens use or trauma to the eye.
Self-care tip from patients
Reducing screen time is indeed helpful for anyone dealing with keratitis — or most other eye conditions — because:
- Looking at screens for long stretches dries the eyes and slows blinking.
- Bright light from phones, laptops, and TVs can worsen photophobia (light sensitivity).
- Eye strain from focusing on small text can aggravate pain or trigger headaches.
If someone has to use a device while recovering, a few tips can make it easier:
- Keep screen brightness low and avoid glare.
- Use larger text size and dark-mode if comfortable.
- Take frequent breaks (20-20-20 rule: every 20 minutes, look 20 feet away for 20 seconds).
- Use preservative-free lubricating eye drops as advised by the doctor.